Schedule An Appointment With Us
Are Your Symptoms Affecting Your Quality Of Life?
Consult our MOH-accredited orthopaedic specialist for an accurate diagnosis & personalised treatment plan today.

MBBS (S’PORE)
MRCS (Ireland)
MMed (Ortho)
FRCSEd (Ortho)
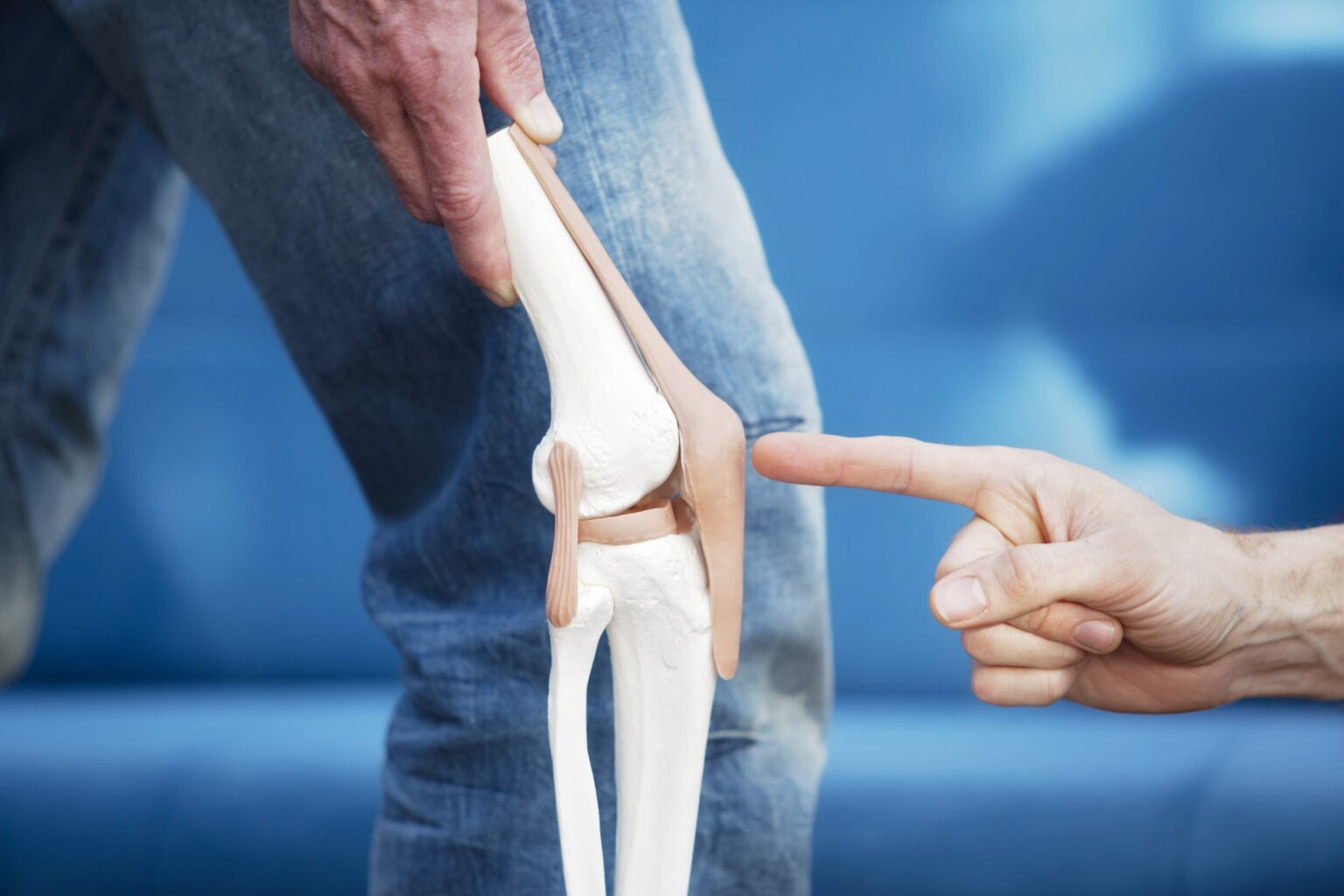
Patella (commonly known as the kneecap) instability and dislocations occur when the patella moves out of its normal position in the trochlear groove, leading to discomfort and impaired knee function. This condition can be acute, resulting from a specific injury, or chronic, due to an underlying weakness in the knee structure.
Patella instability is a significant concern as it can affect an individual’s ability to perform daily activities and participate in sports.
The causes of patella dislocations are multifaceted and are attributed to several factors such as:
Common symptoms that follow after a knee dislocation include:
Chronic instability symptoms emerge gradually and typically involve:


Schedule An Appointment With Us
Consult our MOH-accredited orthopaedic specialist for an accurate diagnosis & personalised treatment plan today.
Diagnosis of Patella Instability and Dislocation includes a detailed evaluation to accurately identify the cause and extent of the injury.
Non-surgical treatment options aim to manage symptoms and support natural healing processes.
Surgical interventions focus on addressing the structural causes of instability to improve knee function.
Involves cutting tight ligaments on the outer side of the knee to allow the patella to realign properly within its groove.
The MPFL is often torn during a dislocation. Reconstruction involves using a graft to replace the damaged ligament and securing the patella in its proper track.
This procedure realigns the patella by moving the attachment point of the patellar tendon on the tibia. It is particularly useful for patients with high-riding patella (patella alta) or those with significant alignment issues.
In cases where the trochlear groove is too shallow or deformed, this procedure deepens the groove to provide a more stable path for the patella.

MBBS (S’pore)
MRCS (Ireland)
MMed (Ortho)
FRCSEd (Ortho)
Dr Kau (许医生) is a Fellowship trained Orthopaedic Surgeon with a subspecialty interest in Hip and Knee surgery and has been in practice for more than 15 years.
He is experienced in trauma and fracture management, sports injuries, and joint replacement surgery.
Prevention strategies are designed to strengthen the knee and reduce the risk of future dislocations.
For Singaporeans, Singapore Permanent Residents and Foreigners.
Please speak to our friendly clinic staff about using your insurance plans.

If you have any enquiry, please do get in touch. Leave us a message and we will get back to you shortly.
After a patella dislocation, it’s important to apply the RICE method – Rest, Ice, Compression, and Elevation – to reduce swelling and pain. Seeking medical evaluation as soon as possible can help to assess the extent of the injury and plan an appropriate treatment strategy.
Yes, once the patella has dislocated, there’s an increased risk of recurrent dislocations. The risk is higher for individuals with certain anatomical factors or those who do not follow through with the recommended rehabilitation program.
Recovery time varies depending on the severity of the dislocation, the treatment method chosen, and the individual’s commitment to rehabilitation. Non-surgical treatment may require several weeks to months, while surgical recovery can take longer.
Most individuals can return to sports after a patella dislocation, but it depends on the recovery process, the strength and stability of the knee, and the type of sports. A gradual return is recommended to prevent re-injury.